Alzheimer’s is a scary disease that we’ve been fighting with for a very long time now. Up till now, we’ve been unable in successfully tackling this disease. However, a recent finding involving gum disease bacteria might just help us solve the Alzheimer problem at long last. The number of cases involving Alzheimer’s have really gone up in the past decade. This disease is known for its agonizingly slow degradation of one’s mental state. We know that people who have Alzheimer’s experience a degradation in parts of their brain. This inhibits their ability to function and basically ruins their lives.
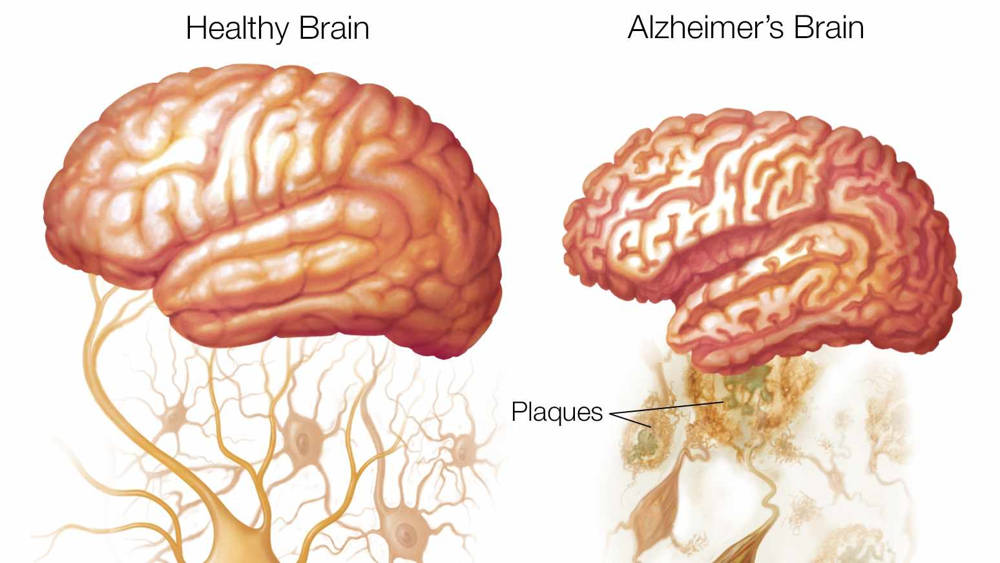
Ever since 1984, we’ve believed that Alzheimer’s is caused by the improper regulation of two protein types present in our brains. Tau and Amyloid proteins exist in large quantities in the brains of people who have been affected by Alzheimer’s. These protein forms large plaques within the brain that we know have a relation to Alzheimer’s disease. Researchers have been sticking to this hypothesis for a long time now. Loads of resources have been invested in Alzheimer research with next to little progress.
Back in 2016, it was discovered that the plaque formed in Alzheimer affected brains served a purpose. It acted as a defence against bacteria present in the brain. There has been a lot of debate regarding this bacteria. Some say that this bacteria is what causes Alzheimer’s while others blame the amyloid plaque. More recent findings have begun producing evidence that goes against the amyloid hypothesis. This research points out that the accumulation of amyloids in the brain may in fact be a result of Alzheimer’s.
Researchers from a number of universities have recently reported the presence of toxic enzymes that are evidence of P.gingivalis activity in Alzheimer affected brains. P.gingivalis is a bacteria that is responsible for gum disease and is known for eating human tissue. Samples taken from numerous Alzheimer affected patients are all riddled with the presence of this bacteria.
Research done on genetically engineered mice has shone even more light on this topic. Scientists observed that when P.gingivalis was injected into mice brains, their brains suffered from inflammation. As a reaction to this, their body began forming amyloid plaque overnight. This formation of plaque in the brain was followed by other symptoms and traits that are commonly observed in Alzheimer affected brains.
Overall, new research has brought forth evidence that may topple the amyloid hypothesis. P.gingivalis reaches the brain through one’s mouth. This bacteria begins thriving in one’s mouth when a sufficient amount of plaque has formed in the gums. It is from here that the bacteria eventually enters into the brain. Once P.gingivalis reaches the brain, your body’s defence mechanism begins producing amyloid plaque that gradually accumulates over the years. The gradual accumulation of this protein in the brain results in one’s cognitive sections of the brain becoming compromised. With this new bit of information, we may be able to find a possible treatment for Alzheimer’s in the near future.