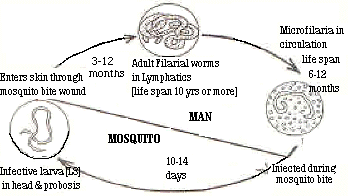
A major public health problem
Human
lymphatic filariasis is caused by the infection with major
nematode parasites Wuchereria
bancrofti and Brugia malayi.
The disease is quite
prevalent in the developing tropical countries.
About 120 million people are infected
all over the world, of which 43
million are affected with
overt physical disabilities from filarial infection.
In India around 412 million people are living in
bancroftian endemic areas with 31 million people are estimated to
be harbouring microfilariae and about 20 million people suffer from
clinical manifestations of the disease, with about 7.5
million of lymphoedema cases and 13 million of hydrocele cases (1).
Further, millions suffer with occult filarial infection in endemic
areas without diagnosis. Filariasis
is prevalent in all states and union teritories except Jammu &
Kashmir, Himachal pradesh, Punjab, Hariana,Rajasthan,Meghalaya,Mizoram,
Nagaland, Manipur, Tripura & Sikkim.
Although
the disease is never directly fatal, it is a debilitating one responsible
for considerable morbidity and social stigma. In 1995, the World Health
Organization (WHO) identified filariasis as world’s second leading cause
of permanent and long term disability next only to mood affecting
disorders (2). The global burden of lymphatic filariasis was estimated to
be at least 850,000 DALYS (Disability Adjusted Life Years Lost) and India
contributes 38% of the global disease burden. In endemic areas out of 1500
million children in the age group of 0-14 years,14 million harbour
microfilaraemia, while 1 million suffer with lymphoedema and 2 million
with hydrocele.
|
|
Wide spectrum of clinical
manifestations in filariasis which need diagnosis and OpDEC therapy*
Acute
& Chronic
* Fever with chills
and rigors
* Lymphoedema with
pain
* Lymphadenopathy
(Cervical, Axillary, Inguinal& Generalised)
* Chyluria /
Haematuria
* Funiculitis
* Epididymoorchitis
* Hydrocele
* Elephantiasis
Occult
* Pulmonary
eosinophilia
* Mono
& Polyarthritis
* Tenosynovitis
* Glomerulo
nephropathy
* Retroperitoneal lymphangitis
(Acute abdomen)
* Central
serous retinopathy
*
Iridocyclitis,
recurrent
scleritis
&
macular oedema
* Endomyocardial
fibrosis
* Urticaria
* Recurrent URI
* Asthmatic
bronchitis
*
Optimal DEC therapy (6mg / kg body wt / day for 21 days each month for
3-12 months). The period
of DEC
treatment is determined based on
immunomonitoring of infection.
|