|
Tuberculosis
Historical
Background : Present
Scenario : Global
Emergency :
Although tuberculosis is
a curable
and to some extent preventable disease, its diagnosis
sometimes, especially in Extrapulmonary tuberculosis, HIV- TB,
Childhood TB, Smear Negative Pulmonary TB becomes difficult.
The WHO declared tuberculosis as a Global Emergency in 1993. Clinical Presentation of Tuberculosis :
The incidence of
pulmonary tuberculosis
is more frequent than extrapulmonary form of tuberculosis (EPTB).
EPTB is increasingly recognized since last decade because of the
emergence of AIDS. Tuberculosis is an air borne disease,
being transmitted via respiratory route on inhalation or ingestion
of droplet nuclei containing varying
quantities of M
tuberculosis bacilli.
The man with active disease when coughs, sneezes or spits,
aerosolizes droplet nuclei. The risk of infection progressing
to disease varies with age, the risk being greatest in children
below 3 years, followed by young adult and the elderly people. Pulmonary
tuberculosis :
This is the most common
form
and affects the lung. The onset is usually insidious and illness
remains unnoticed by the patients for some time. It reaches
full extent with in few weeks. The extent of the disease varies from
minimal infiltrates that produce no clinical
illness to massive involvement with extensive cavitation and debilitating
constitutional and respiratory symptoms. In the absence of effective
therapy, this pursues a chronic and progressive course with
growing bacterial colony. With the progression of pulmonary disease
the normal pulmonary architecture is lost. The over all death rate
of untreated pulmonary tuberculosis approaches 60%. Extra
pulmonary tuberculosis :
This occurs following haematogenous
and lymphatic dissemination of tubercle bacilli from
primary pulmonary infection or a reactivated focus elsewhere
in the body i.e. infected lymph node etc. Number of tissues or
different organs may be infected such as :
involve
the unilateral cervical nodes especially
those high in the neck are more frequent in children. This
form of tuberculosis is the most common form of extrapulmonary
tuberculosis constituting towards 30%
of the total disease. As the disease progresses, sinus tracts are
resulted. These may slowly respond to medication, rarely may require
excision.
is
more common in elderly, although seen in all ages. The involvement
is usually a late manifestation of haematogenous spread of this
disease. The site most frequently involved is the vertebral body
representing 36- 50% of the total bone and joint tuberculosis cases.
Lumbar and low dorsal spines are commonly involved in older; high dorsal
in young. The weight bearing bones / joints (knee, 12-15%) are also
involved. However any bone or joint can be involved. The course
of disease starts from synovial membrane, then
inflammation followed by demineralization and caseous
necrosis.
includes
i) abdominal organ (GIT, liver,
spleen etc.) ii) peritoneum iii) lymphatics. The intestinal
tuberculosis can be related to swallowing sputum tubercule
bacilli or the disease reactivation in peri intestinal
lymphatic tissue. The ileocoecal area of small intestine is
the most common site (91%) involved. Peritoneal TB presents with
seeding of tubercles through out the peritoneal surface and occurs in
ascitic (exudative) or plastic (adhesive or dry) forms. This form of TB is
easily confused with other diseases such as irritable bowel
syndrome, alcoholic cirrhosis etc. Usually the signs and
symptoms are vague and non specific, increases with age and patient
presents with abdominal swelling, vague pain and alternate diarrhoea
and constipation.
is
most common amongst infants, children
with extrapulmonary tuberculosis. The patient presents in
different stages: early fever, headache, and malaise; later
confusion, seizures and coma. The prognosis is related to stage.
is
rare in young, more frequent among females. This may involve
kidneys, ureters, bladder, testes, epididymis, uterus, fallopian
tubes etc. This may complicate to early or late obstructive
uropathy, infertility etc. |
Pleurisy with effusion occurs when the pleural space is seeded with the M tb. bacilli. This may be acute or indolent; severe or asymtomatic.
· Tuberculous
pericarditis represents
as extension of pleurisy. This causes, dyspnoea and vague discomfort.
Exudative effusion occurs and patients present with fever and
pericardial pain, chronic obstructive pericarditis being its last
sequele. · Disseminated tuberculosis is most frequent in very young or old. Chest film abnormalities may lag and patient presents with progressive fever. Early therapy is vital. Diagnostics:
Early diagnosis of
tuberculosis is important both to individuals and to community, and is
very crucial yet difficult to achieve. Presently the diagnosis of
tuberculosis largely depends upon clinical, radiological, cytological
& bacteriological examinations. Though the direct microscopy of
sputum for acid fast bacilli (AFB) is reliable for pulmonary
tuberculosis, it is not that sensitive, limitations being, it may give
false negative results and require a high degree of bacillary load of
50000 bacilli / ml of sputum and is subject to inherent errors like
contamination. Other demerit is that it is positive in open cases only.
Thus it is not helpful in extrapulmonary form of tuberculosis and in
childhood tuberculosis where sputum is not available. The culture method
is cumbersome and time taking, requires 6-8 weeks for positive results.
The radiological examination is non specific and not suitable for field
studies in developing countries, like India. The tuberculin skin test is
not reliable in discriminating active form from non active tuberculosis.
Even the new techniques such as PCR, DNA Probes, RFLP, BECTEC system,
etc. for early diagnosis of tuberculosis are no doubt are sensitive and
help rapid diagnosis, but still do not find their way into routine
diagnosis and more over not cost effective and practical in developing
countries. Thus, there is a search for alternative test which will stand
with its merits in vigorous clinical trails. Serodiagnostics have
attracted considerable attention of the Investigators. Immunodiagnosis:
SEVA TB ELISA (IgG &
Ag) system based on the detection of tubercular IgG antibodies and
antigen in tuberculosis has been developed and explored in several ways
at this institute. The detection of IgG antibody (titre 1:600 and above)
by indirect ELISA against SEVA TB ES 31/41 antigen in pulmonary and
extra pulmonary tuberculosis suggests active tuberculosis infection.
Free tubercular & Immune complexed antigen (IC-AG) is detected using
affinity-purified anti ES-31 antibody by sandwich ELISA. A serum with an
antigen titre of 1:300 and above is considered for positive reaction.
The combination of antibody, free and IC-Ag detects 100% cases of
pulmonary TB. The test is quite helpful in childhood tuberculosis where
it is difficult to obtain sputum sample. This test has been found useful
in clinically suspected and anti tuberculosis therapy (ATT) responded
cases, which were negative for bacterial examination. This test has also
been useful in confirming tubercular aetiology in extra-pulmonary
tuberculosis (bone & joint, abdominal, CNS-meninges, lymph node,
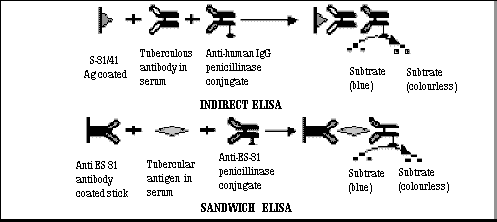
genito-urinary etc.) Antibody
detection by indirect penicillinase ELISA and Antigen detection by
Sandwich ELISA:
The antibody detection
test is based on the detection of spec-ific IgG antibody to purified
culture filtrate antigen of Mycobac-terium
tuberculosis H37Ra (SEVA TB ES
31/41) by indirect penicil-linase ELISA. The ES-31/41 antigen co-ated
CAM sticks are incubated with diluted human sera followed by addition of
antihuman IgG penicill-inase conjugate. After washing, the enzyme
reaction is detected using starch-iodine-penicillin 'V'
substrate. The disappea-rance of blue color of substrate indicates the
presence of antibody to ES-31/41 antigen. In a study on antibody
detection to SEVA TB ES-31 has given a sensi-tivity of 92% compared to
sputum AFB positivity of samples tested and a specificity of 95% in
pul-monary tuberculosis (Banerjee et
al 2001). Antibody detection to ES- 41 was found to be quite useful
in diagnosis of bone & joint and abdominal tuberculosis. The
free and IC-Ag dete-ction is done by sandwich ELISA. The CAM sticks
sensitized with affinity purified goat antibody aga-inst M.tb
ES-31 antigen are incubated with appropriate test sera followed by
addition of penicillinase labeled anti ES-31 antibody. The positive
reaction is detected by disappearance of blue color of the substrate.
Free antigen and IC-Ag detection assays have given sensitivity of 80%
& 72% respectively and specificity of 95% & 97% respectively.
This test is quite helpful to detect tubercular IgG antibodies in extra
pulmonary tuberculosis cases viz; tubercular lymphadenopathy(88%),
tubercular meningitis (90%), abdominal tuberculosis (82%), bone &
joint tuberculosis (85%), genitourinary tuberculosis (71%) etc. (Banerjee
et al, in communication). Immunomonitoring:
A follow up study of immune status during the course of ATT of
tuberculosis patients showed an initial rise of tubercular antibodies in
the first month of treatment followed by gradual decrease in the titers
by the end of treatment. Similarly circulating tubercular antigen levels
were also found to be decreasing gradually with the treatment. At the
end of six months of ATT, about 75% showed the absence of circulating
tubercular antigen. Thus presence of antigen may be used as a marker for
elimination of tuberculosis infection as well as compliance of the
patients with ATT.
|
|
|
|
||